SKILLED NURSING
Predictive analytics for PDPM, Quality Measures and MDS
SimpleAnalyzer™ is the leading solution for real-time improvement in MDS outcomes and quality.
SimpleAnalyzer™ – trusted by thousands of SNFs
Use real-time, predictive MDS analytics to optimize PDPM, improve compliance and simplify workflow.
Improve MDS accuracy.
See what CMS sees before they see it. Pinpoint problems and make corrections in real time. Benchmark your data against 5,000+ providers.
Predict Five-Star/QM outcomes.
Predict quality ratings months in advance. Proactively spot negative trends so you can easily make real-time improvements.
Optimize PDPM reimbursement.
Leverage MDS clinical intelligence to gain visibility into PDPM. View financial impact by resident/facility and optimize ICD-10 coding.
Automate MDS transmission workflow.
Automatically transmit MDS batches to CMS iQIES and retrieve CASPER reports in one simple dashboard.

When I saw the SimpleAnalyzer dashboard, I truly got so excited. It is simply one of the BEST programs I’ve seen.
Real-time analytics make the difference
Get instant insights to proactively improve PDPM and Five-Star/Quality Measure ratings.
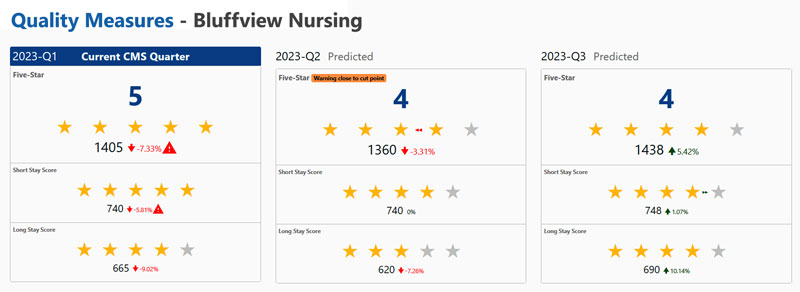
Predict Five-Star and Quality Measure ratings.
Why wait for retroactive CMS data? Proactively spot trends in real time and make improvements before ratings are affected.
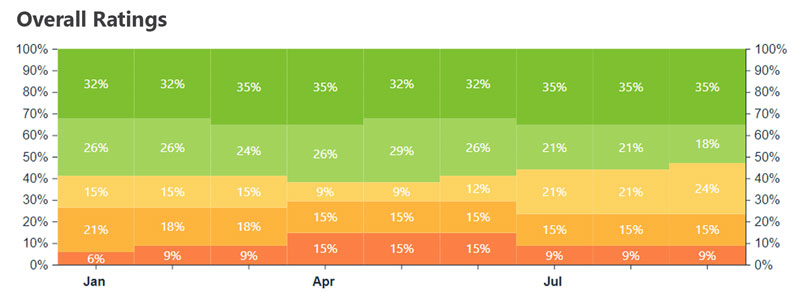
Quickly improve quality outcomes.
Monitor trends and predict rating changes. Review data by survey, staffing or quality. Easily monitor multiple facilities.
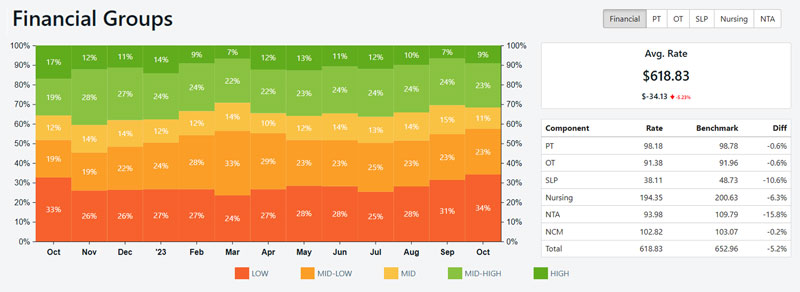
Maximize PDPM financial performance.
Optimize ICD-10 coding practices, monitor financial impact by facility/resident, and customize PDPM rules to your needs.
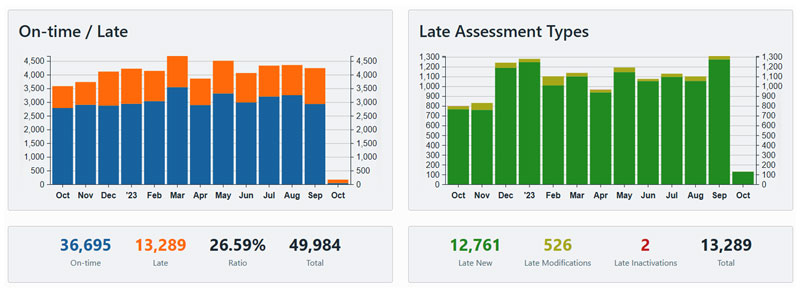
Improve MDS accuracy – proactively.
MDS transmission and CASPER reporting are built into the workflow, so you have real-time control and access to all your information.
Master PDPM with powerful, predictive analytics
Create a PDPM-centric workflow using intuitive forecasting tools and proactive analytics.

Forecast PDPM reimbursement.
Predict reimbursement for all case-mix groups by population. Analyze trends over time and optimize workflow to increase PDPM revenue.
Predict revenue by resident/facility.
View primary diagnoses, default clinical category and case-mix index rates for every resident. Proactively identify and fix errors to maximize PDPM potential.
Identify PDPM diagnoses by resident.
Monitor multiple clinical categories by resident and facility. Quickly identify invalid or inaccurate diagnoses that may lead to missed billable opportunities.
Compare PDPM impact across facilities.
View residents with invalid diagnoses and average case-mix index by facility. Explore MDS data to highlight areas of clinical complexity and risk.
Improve outcomes while simplifying workflow
Take control of PDPM, quality outcomes and MDS workflow with one simple tool.
Optimize ICD-10 coding practices.
Analyze diagnoses to ensure compliance and maximize reimbursement. Monitor comorbidities and scan for valid diagnoses and clinical categories.
Customize scrubber rules by facility.
Design your own analysis policy and staff roles, down to individual facilities. Customize rules to your workflow to minimize false alerts and email fatigue.
Reduce rehospitalizations.
Quickly diagnose episode/stay irregularities and optimize clinical outcomes. Compare multiple facilities to pinpoint residents needing immediate attention.
Maximize state incentive payouts.
SimpleAnalyzer™ provides in-depth, state-level analytics for SNFs in states with quality incentive programs. Currently available for California, Florida, Ohio and Texas.
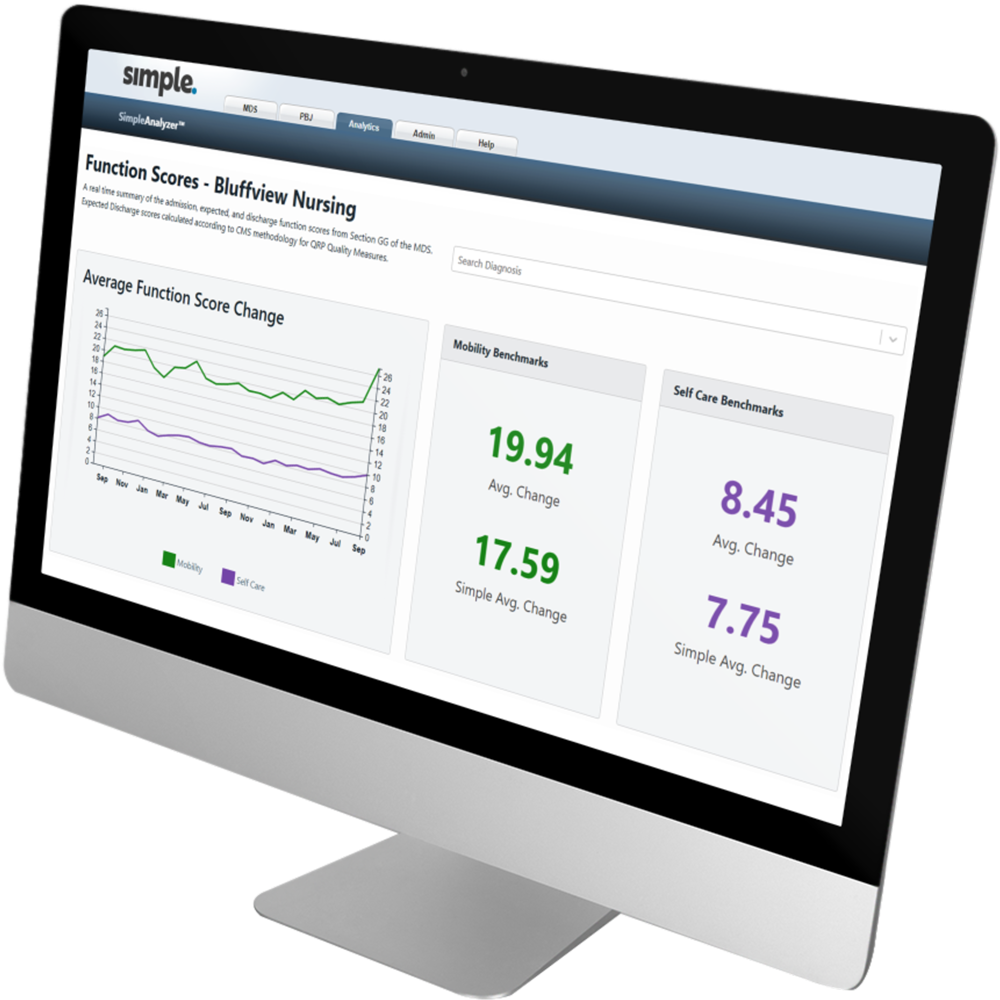
Get your SimpleAnalyzer™ demo
Taking charge of PDPM and Quality Measures is simple.
SimpleAnalyzer is trusted by thousands of SNFs as a vital element of their reimbursement strategy and MDS workflow. Find out why with a free online demo.




