Predictive analytics for MDS, PBJ, Claims and OASIS
Post-acute compliance has never been simpler.
Use real-time data to improve compliance, optimize reimbursement and maximize clinical outcomes — with one simple solution suite.
LATEST POSTS
![Featured image for “[Free webinar] HOPE on the horizon: Clinical accuracy & practical strategies for HOPE Compliance in 2025”](https://www.simpleltc.com/wp-content/uploads/2024/12/Simple-webinar-HOPE-on-the-Horizon-Jan-2025.png)
[Free webinar] HOPE on the horizon: Clinical accuracy & practical strategies for HOPE Compliance in 2025
![Featured image for “[Webinar recording] Elevate Your Five-Star: Hidden SNF Insights for Health Inspections, Staffing & Quality”](https://www.simpleltc.com/wp-content/uploads/2024/12/Simple-webinar-recording-Elevate-Your-Five-Star-Dec-2024-v2.png)
[Webinar recording] Elevate Your Five-Star: Hidden SNF Insights for Health Inspections, Staffing & Quality
![Featured image for “[On-demand] CHANGE AHEAD: How the Election Could Shape Healthcare and Long-Term Care”](https://www.simpleltc.com/wp-content/uploads/2024/11/Simple-webinar-recording-Change-Ahead-ADVION-Nov-2024.png)
[On-demand] CHANGE AHEAD: How the Election Could Shape Healthcare and Long-Term Care
![Featured image for “[On-demand] Quarterly PBJ Webinar – Q4 2024 Edition”](https://www.simpleltc.com/wp-content/uploads/2024/11/Simple-recording-Quarterly-PBJ-Webinar-Q4-2024.png)
[On-demand] Quarterly PBJ Webinar – Q4 2024 Edition
SOLUTIONS
Predictive analytics for skilled nursing
The industry’s leading compliance suite for MDS 3.0, Payroll-Based Journal (PBJ) and Claims analytics.
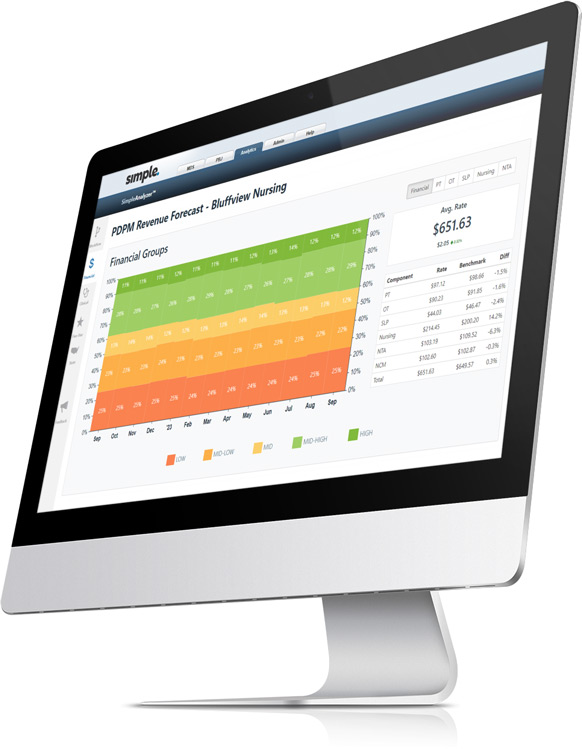
SimpleComplete™: Your complete solution for SNF reimbursement, referrals and regulatory compliance.
- SimpleAnalyzer™: Quickly improve PDPM, Five-Star, QMs, and iQIES workflow with predictive MDS analytics.
SimplePBJ™: Assemble, validate and submit Payroll-Based Journal, plus optimize Staffing Five-Star.
- CORE Analytics™: Optimize PDPM outcomes and minimize audit risk through real-time Claims analysis.
OASIS-E compliance for home health
One simple solution to analyze, scrub and submit accurate OASIS-E files.
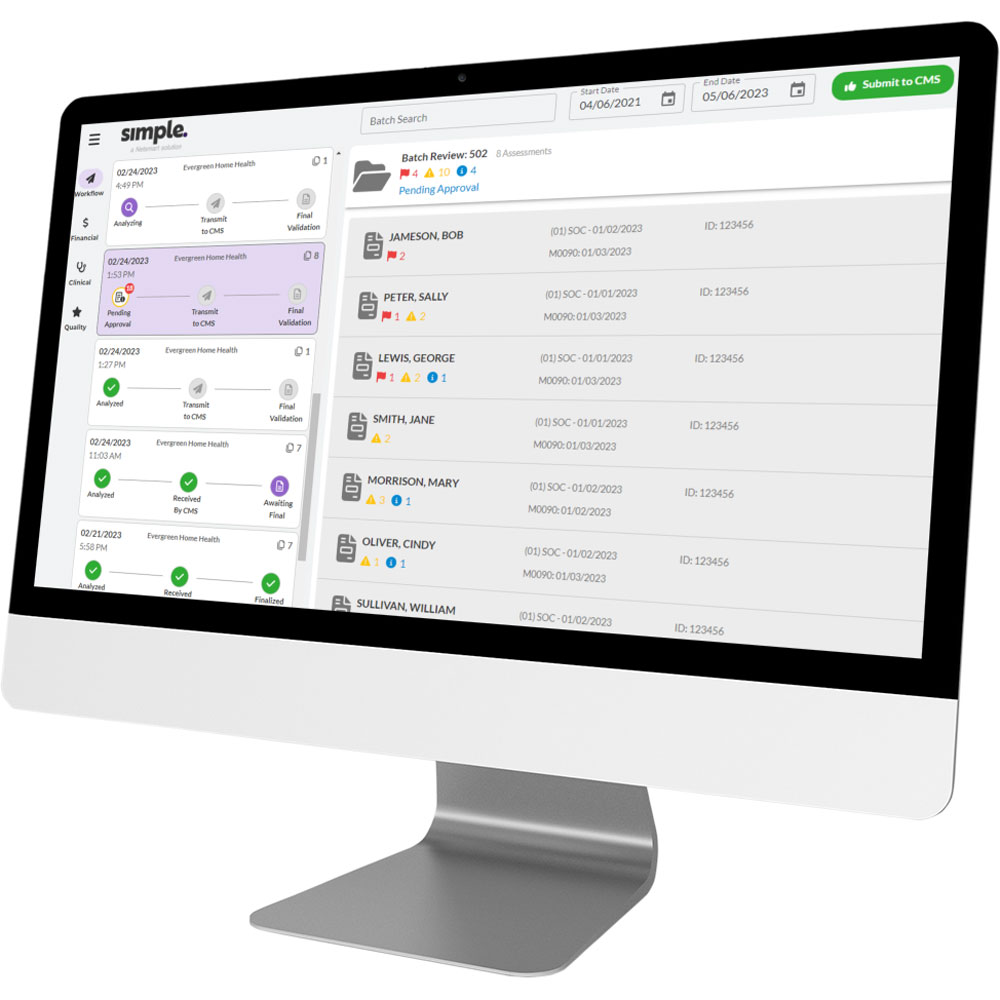
- OASIS-E data scrubbing: Get a clear view of OASIS-E accuracy so you can correct issues in real time.
- iQIES submission: Automatically transmit OASIS-E batches to CMS with no intervention.
Simple rule management: Customize rules and alerts to eliminate errors and regulatory headaches.
- iQIES report center: Easily view CMS reports across all agencies so you can make informed decisions.
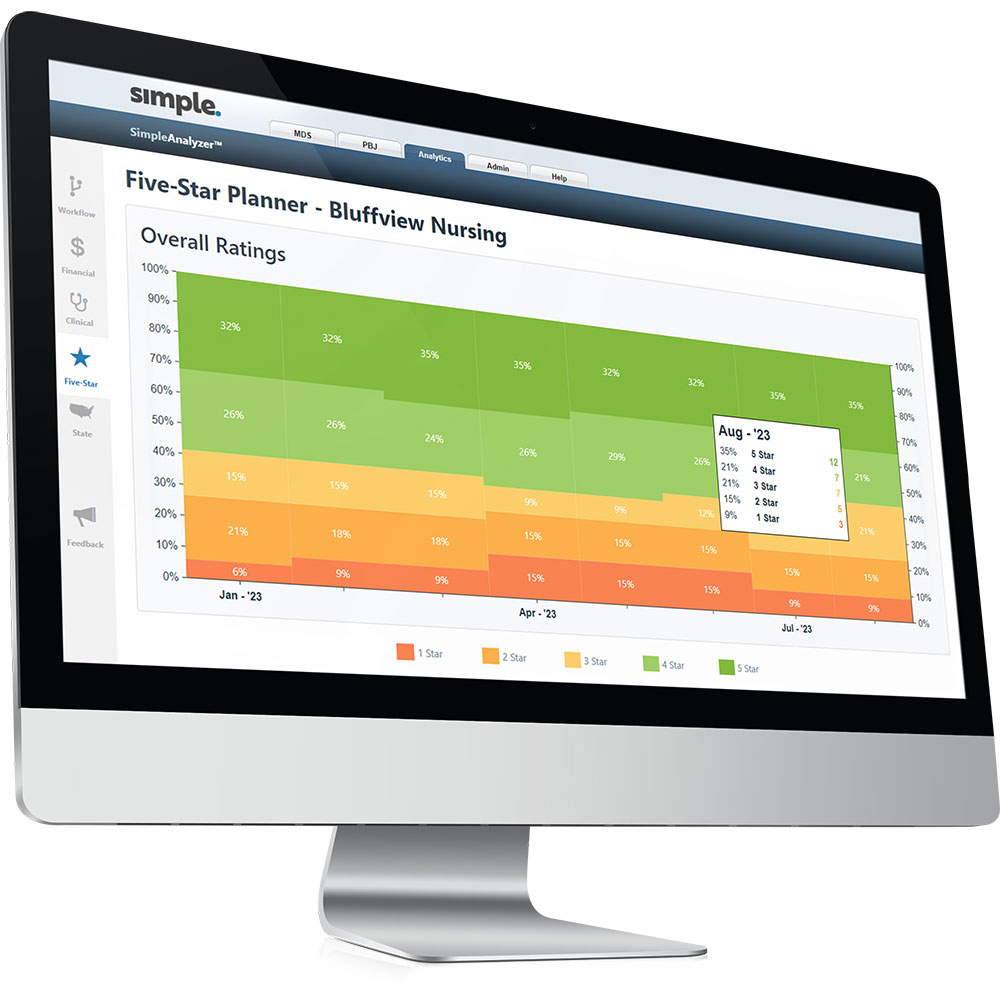
State analytics and quality measures
Optimize critical state incentive measures and payouts, while streamlining forms and compliance processes.
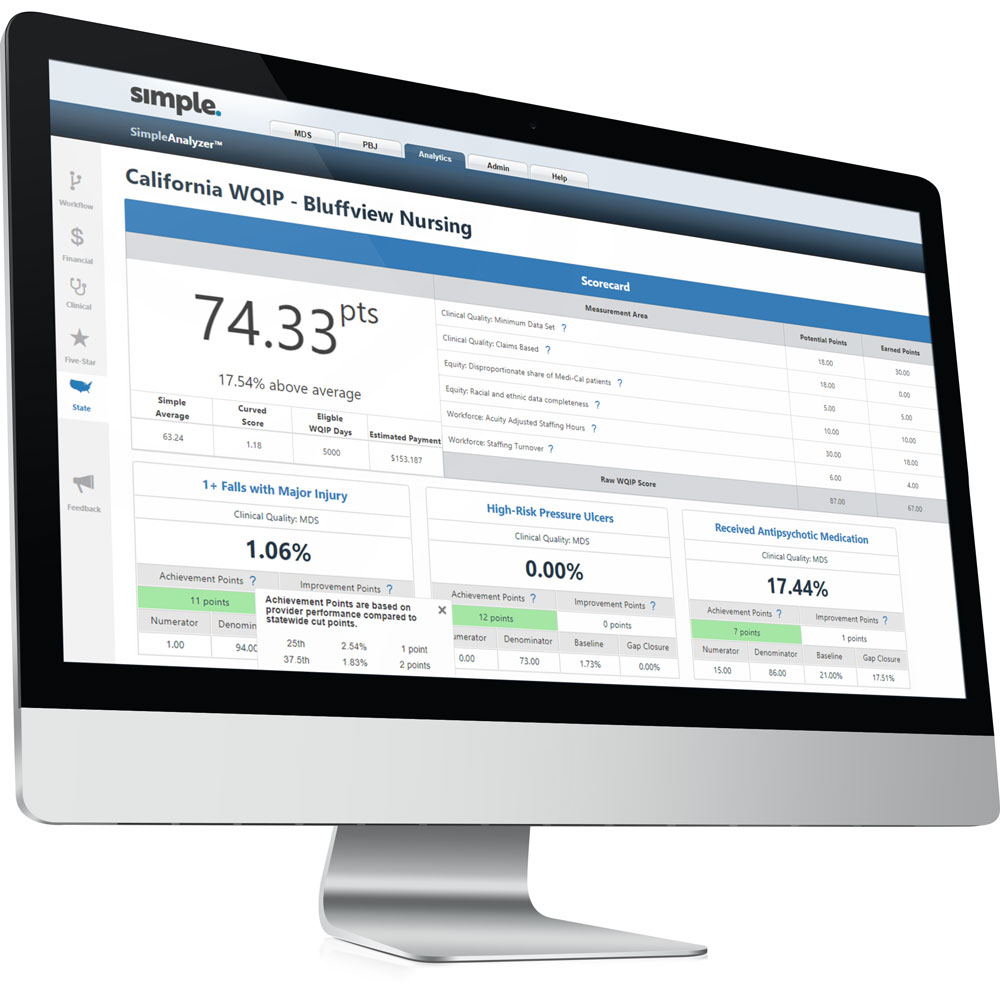
- State quality incentive programs: Predict quality incentive payments by company/facility and improve QMs. (California, Florida, Ohio and Texas.)
- Texas Medicaid and PASRR/LTCMI: Automate LTCMI, 3618/3619, PASRR, MESAV and MCO, simplify Medicaid, and improve reimbursement.
Clients are saying…
Simple has by far been the best industry software company I have ever worked with.
Your staff are awesome, the service is affordable, and it does exactly what it’s designed to do!
Very user-friendly, accurate information, overall makes my job less stressful.
Simple, period
- Simple. Simpler workflow, better reimbursement.
- Trusted. Thousands of providers rely on Simple solutions.
- Cost-effective. Designed to be affordable for any provider.
Smart. Real-time data supports better results.
- Secure. Your data is safe and always available.
Loved. Clients tell us they love Simple solutions.




